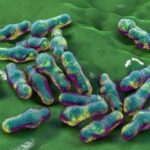
Secondary bacterial infections—such as those caused by Streptococcus pneumoniae and Haemophilus influenzae—are a major cause of death after flu and other respiratory viral infections. Now, researchers have found that a type of gut microbes called segmented filamentous bacteria, or SFB, protect mice from these deadly infections by reprogramming specific immune cells in the lungs.
The findings, published in Science Immunology, suggest that leveraging gut-lung interactions could offer new ways to prevent or reduce severe complications from respiratory viral infections.
One reason people get secondary infections after flu is that the virus damages lung immune cells called alveolar macrophages (AMs). SFB can help AMs stay strong during viral infections, but it’s unknown whether these microbes protect against secondary infections and how they might do so.
Researchers led by Vu Ngo at Georgia State University in Atlanta studied whether SFB protect mice from deadly bacterial infections after flu.
Boosting immunity
The team compared mice with and without SFB in their gut. Animals without SFB lost a lot of AMs and had severe lung infections after flu. In contrast, mice with SFB had strong AMs and showed much less lung damage and fewer bacteria. But when the researchers removed AM cells, even mice with SFB became vulnerable.
Scientists have known that mice typically acquire SFB from their mothers. Compared to pups of mice without SFB, those of mice with SFB had healthier lungs, fewer bacteria, and better survival after flu and bacterial exposure, and this protection lasted for at least four generations.
Further experiments showed that SFB work by reprogramming the lung’s AMs to resist flu-induced damage and remain effective at killing bacteria, rather than by bringing new immune cells into the lungs. The microbes also boost antibacterial activity in immune cells throughout the body.
Transferring protection
Next, the researchers found that AMs from mice without SFB lost function in an inflamed environment, but if they were placed in the lungs of mice with SFB, they regained their antibacterial activity.
Rather than acting only by reducing harmful inflammatory signals, SFB change AMs at the genetic and metabolic level, boosting their ability to kill bacteria, produce immune helpers, and maintain energy. Transplanting AMs from SFB-colonized mice into mice without SFB transferred protection, the researchers found.
“We speculate that defining and subsequently harnessing the mechanism by which SFB colonization reprograms AM will lead to new strategies to mitigate the [respiratory viral infection] induced disease burden,” the authors say.