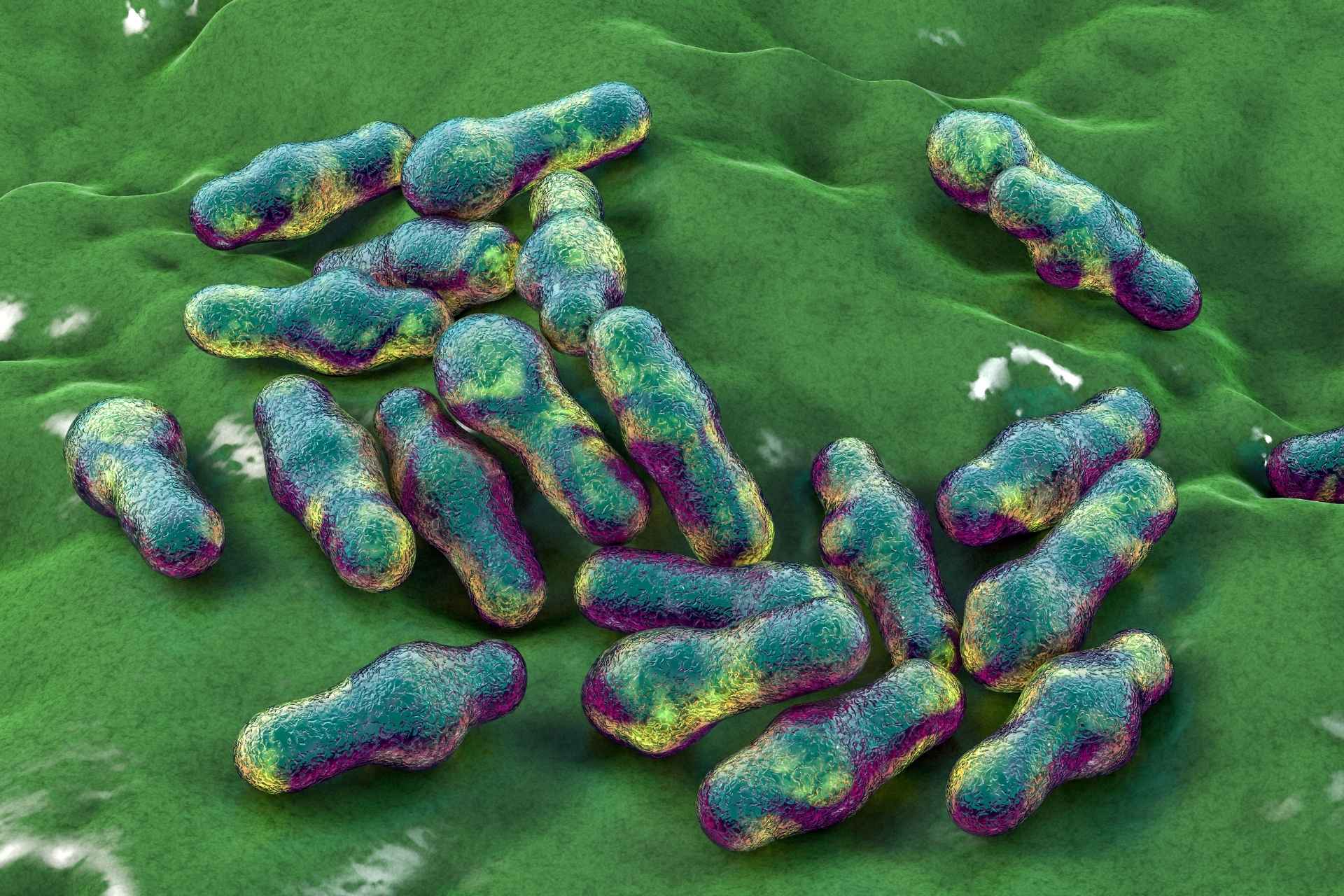
Tiny whip-like structures called flagella, which help bacteria move, can either calm or trigger the immune system. Now, a new study reveals that differences in flagella proteins determine whether gut bacteria keep the immune system in check or drive inflammation linked to Crohn’s disease.
The findings, published in Science Immunology, suggest that gut Clostridia can be divided into two groups, with one group contributing to gut inflammation under certain conditions.
Scientists have known that Clostridia bacteria make proteins called flagellins, which build flagella. Flagellins can also interact with the immune system, with some triggering only weak immune responses and others causing inflammation. However, it’s unclear how differences in flagellin types affect their ability to stimulate the immune system and which flagellins promote or prevent inflammation in the gut.
To address this question, Lennard Duck at the University of Alabama at Birmingham and his colleagues set out to study more than 100,000 bacterial genomes from gut Clostridia.
Immune activation
The researchers found that the genes controlling flagella, called motility genes, are arranged differently across Clostridia bacteria, even among closely related families. Some bacteria, such as Lachnospiraceae, have multiple motility genes and more diverse flagellins, while others have fewer of these genes and less diversity.
Based on flagellin diversity and motility gene organization, the team classified gut Clostridia into two groups, G1 and G2. Next, they tested these two groups of bacteria in germ-free mice to see how they affect the gut.
Both groups could colonize the gut, boost protective immune cells, and stimulate the production of antibodies that help maintain normal gut balance. However, G2 bacteria triggered stronger responses in gut cells, including genes linked to inflammation and stress, while G1 bacteria mainly activated protective functions.
Gut inflammation
When the gut’s barrier was weakened, G2 bacteria—but not G1 bacteria—caused inflammation and tissue damage in the colon lining. The researchers found that flagellins differ between G1 and G2 gut bacteria: Most G1 bacteria produce flagellins at very low levels, while G2 bacteria produce flagellins that strongly activate the immune system. What’s more, G2 flagellins stimulate inflammatory signals, whereas G1 flagellins don’t.
In people with Crohn’s disease, G1 bacteria are typically reduced, while G2 bacteria are more abundant in inflamed tissues, the researchers also found. This finding, they say, suggests that the balance between G1 and G2 bacteria and their flagellins may influence gut inflammation and disease.
“This study identified key features of specific commensal bacteria that have colitogenic potential and revealed one mechanism whereby these organisms can potentially initiate intestinal inflammation,” the authors say.