• Immune reaction
• Microbiota modulation
What is already known on this topic
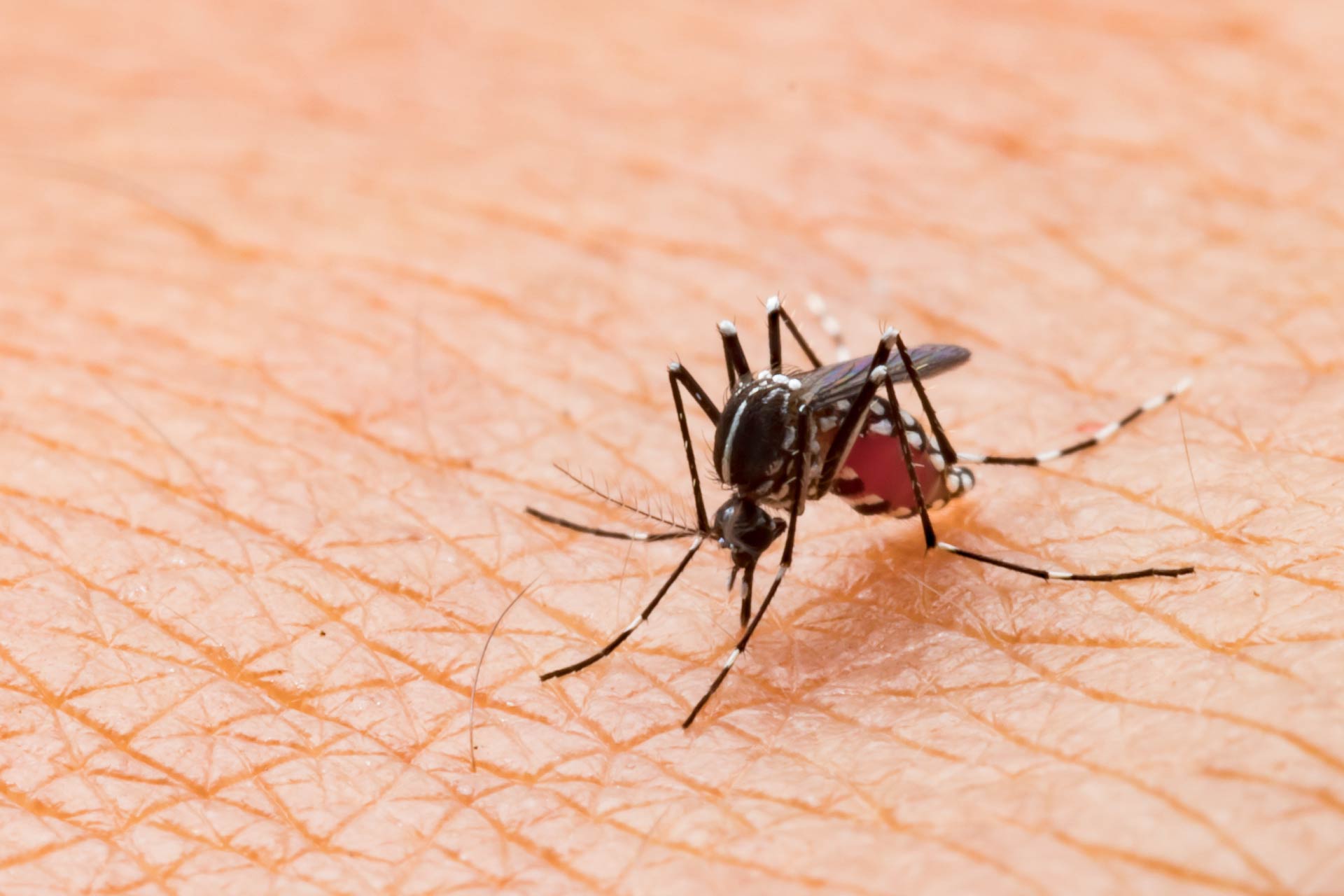
Malaria is a life-threatening, mosquito-borne disease caused by Plasmodium species, a type of single-celled parasites. Every year, Plasmodium infections cause more than 200 million cases of malaria and about 1 million deaths. Studies have shown that gut microbiota composition can influence malaria severity, but little is understood about the underlying mechanism.What this research adds
A study in mice shows that gut microbiota composition can influence the host’s immune response, driving differences in the number and activity of antibodies against the Plasmodium parasite. These changes also affect the ability of the immune system to remember the pathogen and help to mount a faster defense if the parasite invades again.Conclusion
The findings could lead to the development of treatment approaches for malaria.
Every year, infections by malaria parasites cause more than 200 million cases of the disease and about 1 million deaths. A new study in mice shows that the gut microbiota composition can influence mice’s immune response during infection with malaria parasites.
The findings, published in Cell Reports, could lead to the development of treatment approaches for malaria.
Malaria is a life-threatening, mosquito-borne disease caused by Plasmodium species, a type of single-celled parasites. Previous studies have shown that gut microbiota composition can influence malaria severity. In particular, scientists know that mice from different vendors exhibit profound differences in their susceptibility to infection with a certain Plasmodium species called P. yoelii. Susceptible mice show signs of weight loss or mortality, whereas resistant mice do not. However, the mechanism underlying these differences have remained elusive.
To better understand the role of gut bacteria during Plasmodium infections, Nathan Schmidt at Indiana University School of Medicine and his colleagues infected ‘resistant’ and ‘susceptible’ mice with P. yoelii.
Immune reaction
Specific types of immune T cells are necessary for a process called germinal center (GC) reaction, and they provide signals for another type of immune cells, known as GC B cells, to develop into long-lived antibody-producing cells and memory B cells. These cells allow the immune system to remember a pathogen they’ve encountered and help to mount a faster defense if the pathogen invades again.
Compared to susceptible mice, resistant animals show an increased expansion of GC B cell populations, as well as heightened levels of parasite-specific antibodies. These immune responses allowed the rodents to successfully fight P. yoelii infection.
Following Plasmodium infection, mice’s spleens usually become dark and become nearly 10 times heavier than spleens of uninfected mice. The researchers found that, seven days after infection, distinct GC-like sections were evident in the spleens of both resistant and susceptible mice. But resistant mice had distinct GC-like sections in their spleen for up to 11 days, whereas susceptible ones don’t, which suggests that the increased levels of antibodies and GC B cells observed in resistant rodents are a result of the animals’ ability to maintain GC-like structures for longer.
Microbiota modulation
The team found that germ-free mice colonized with gut bacteria from resistant mice became resistant to Plasmodium infection, whereas those that were colonized with the microbiota from susceptible mice became susceptible to infection. Further experiments showed that the microbiota composition affects the expansion of GC B cells and the levels of parasite-specific antibodies, likely by regulating GC reactions to control the parasite burden.
Gut microbiota-induced resistance to infection with P. yoelii also results in better survival in mice infected with P. berghei, a parasite that causes malaria in rodents. Overall, resistant mice showed increased interactions between T and B cells and improved B cell functionality, the researchers found.
“This study uniquely demonstrates that the composition of gut microbiota influences the overall magnitude and quality of GC reactions and thus the severity of an infectious disease, including memory development and protection from re-infection,” the researchers say.
Although the molecular relationship between the gut microbiota and the immune response has yet to be elucidated, the findings suggest that modulating the gut microbiota could help to increase Plasmodium-specific immunity, thus reducing disease severity and malaria-associated mortality, the researchers say.